AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Resonance lung sounds4/7/2024 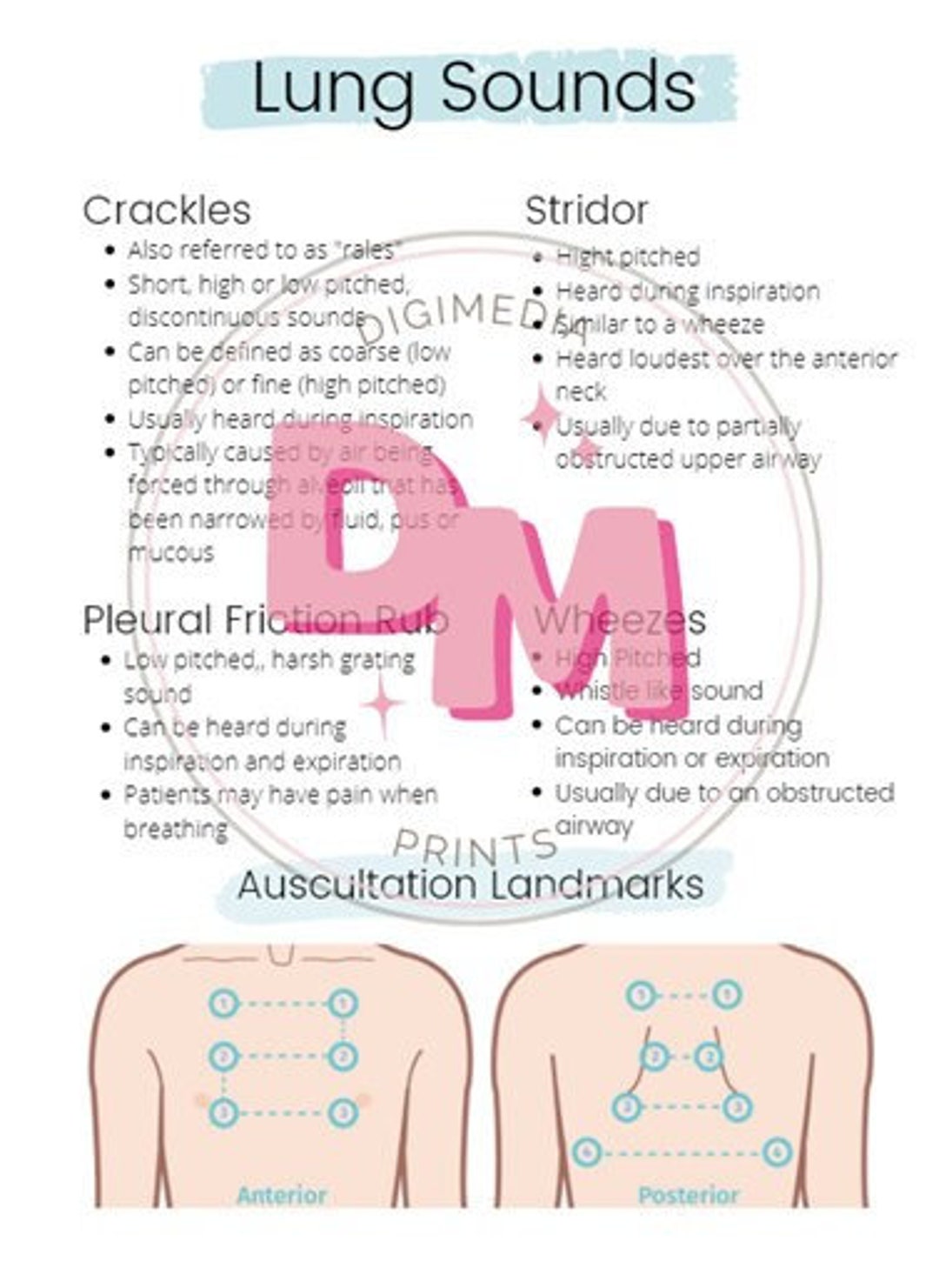
Focus on breath sounds first only then on adventitious sounds. Listen to and compare identical places on each sides. At each place listen to at least one complete breath cycle. The key is to listen to the all of the chest. Listen to the front or back of the chest first, from apex to base or vice versa based on your preferences and clinical judgement. 
When listening to the back, ask the patient to cross arms over the chest to evert the shoulder blades. Ask the patient to breathe deeply through the open mouth. Even if it’s not cold it’s a nice gesture of special care. Warm up the cold stethoscope by rubbing the membrane. 
If the patient is not able to sit up, roll the patient to each side to examine the back. Female patients should have only front or back of the chest exposed at once. Room should be quiet and patient sitting up, decently exposed. Any kind.Įxcept for the last step, the sequence is the same as in Lung Auscultation – Normal Breath Sounds. The key to detailed and correct examination is systematic approach. Some physicians prefer to listen back to front, top to bottom or vice versa. There is no best way of listening to the lungs. The physician is listening to the body wall indirectly through the stethoscope which is composed of the bell or membrane, the tubing and the earpieces. It’s the method of auscultation as known today. However, since the discovery of stethoscope this method was replaced by more accurate, convenient and hygienic mediate auscultation. In this method the physician is listening to the body wall directly with the unaided ear. There are two methods of auscultation – the immediate and mediate auscultation. In 2000 the European Respiratory Society defined lung sounds based on their computerized analysis. In 1977 the American Thoracic Society proposed the terminology that was later in 1987 presented at the symposium of the International Lung Sounds Association and adopted for clinical practice. Studies show physicians use up to 16 different terms to describe similar sounds. However, all the terms are still used today in medical textbooks and clinical practice as well. To distinguish them he used adjectives like “moist”, “dry”, “crepitus” or “sibilus”, only to substitute it later for rhonchus so the patient would not mistake it for death rattle.Īt later date terms wheeze and crackle were introduced, proposed for continuous musical and discontinuous sound, respectively, replacing the old rale and rhonchus. He identified five adventitious sounds and all of them called rales (from French word râle – to rattle). The first one to describe auscultatory findings was René Laennec, the inventor of stethoscope, in his monography A Treatise on the Disease of the Chest and on Mediate Auscultation. Lung Auscultation – Adventitious Breath Sounds.Lung Auscultation – Normal Breath Sounds.Over the stomach, but is not a normal chest sound. Sounds are hollow, high, drumlike sounds. An area of hyperresonance on one side of the chest With air, such as may occur in patients with COPD, or patients having anĪcute asthmatic attack. Hyperresonant sounds may also be heard when percussing lungs hyperinflated Normally heard when percussing the chests of children and very thin adults. Sounds that are louder and lower pitched than resonant sounds are Replaces air-containing lung tissues, such as occurs with pneumonia, pleural Dullness replaces resonance when fluid or solid tissue Or thudlike sounds are normally heard over dense areas such as Or extremely dull sounds are normally heard over solid areas such Sounds are low pitched, hollow sounds heard over normal lung tissue. Look at the following diagram that shows percussion notes on the posterior chest: Visualize the structures underneath as you proceed. Work from the top part of the chest downward, comparing sounds heard on both the right and left sides of the chest. Then, strike the finger placed on the patient's skin with the end of the middle finger of your dominant hand. Place the first part of the middle finger of your nondominant hand firmly on the patient's skin. Percussing the anterior chest is most easily done with the patient lying supine the patient should sit when percussing the posterior chest. Percussion helps to determine whether the underlying tissues are filled with air, fluid, or solid material. Percussion sets the chest wall and underlying tissues into motion, producing audible sounds and palpable vibrations. Just as lightly tapping on a container with your hands produces various sounds, so tapping on the chest wall produces sounds based on the amount of air in the lungs. Percussion is an assessment technique which produces sounds by the examiner tapping on the patient's chest wall.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
